By Dr. Nicole Sundene
Author of "The Hormonal Acne Diet"
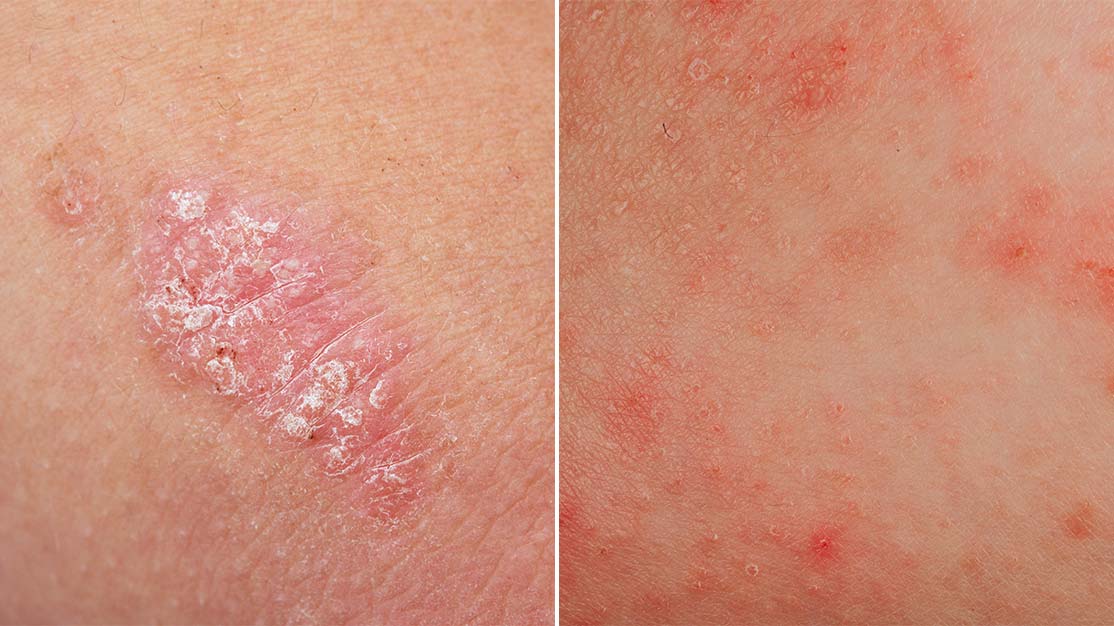
Eczema is a skin condition characterized by redness, dryness, itching, and irritation. Mainly it occurs on the arms, inner elbows, knees, back, and head area, but remember that it can affect any skin area. The eczema symptoms may flare up, subsides, and repeat at different intervals. Studies reported that eczema is 15-30% prevalent in children and 2-10% in adults. [1]
Moreover, eczema is highly prevalent in children compared to males. It is estimated that eczema affected approximately 9.6 million children under the age of 18 in the US. Plus, around 31.6 million people in the United States have eczema. Note that eczema occurs in all types of skin, colors, and ethnicities.
Both genetic (mutation in gene Filaggrin) and environmental factors (Irritants and Allergens) are involved in eczema development. Moreover, research studies categorized eczema into seven types based on the area of the skin and symptoms. These include atopic dermatitis (most common form), contact dermatitis, Neurodermatitis, Dyshidrotic eczema, Nummular Eczema, Seborrheic Dermatitis, and Static Dermatitis. [1]
Signs and symptoms of Eczema
Studies reported the following signs and symptoms of eczema that may vary from person to person. [1, 2] These include:
It is important to know that eczema increases the risk of various skin infections caused by bacterial, viral, and fungal pathogens. Also, it negatively impacts daily life activities via sleep disturbance, asthma, and hay fever. [1, 2]
Eczema Diagnosis
There are no specific lab tests and diagnostic techniques for eczema confirmation. The diagnosis involves the evaluation of clinical symptoms such as rash appearance and history. Plus, in some cases, allergy testing and patch testing are also considered for eczema diagnosis. [1, 2]
Eczema Treatment
The treatment of eczema involves the intervention of different therapeutic agents to ease symptoms, prevent a flare-up and improve skin conditions. Both systemic and topical agents are indicated over months or years, depending on the severity of the eczema condition.
Medical research studies reported three treatment approaches for eczema management. [2, 3]
Basic Treatment
Basic treatment involves the application of emollients for the management of skin dryness and pruritus. Emollients restore cutaneous hydration that reduces flaring up the eczema symptoms. Topical emollient decreases dependence on topical steroids. It is important to know that apply emollient on the skin within three minutes of bathing with lukewarm water. The patient can use 250 g of emollients per week as per national institute for health and clinical excellence [NICE] guidelines. The selection of moisturizers depends on the patient's symptoms, skin physiology, and season. [2, 3]
Moreover, always consider other protective measures before the application of emollient. These include a detailed history, allergy tests, and careful evaluation of clinical manifestations to rule out the aggravating factors. Plus, always prefer wool clothing over nylon dressings as wool quickly absorbs sweat and prevents skin scratching. Remember that certain perfume ingredients can also aggravate eczema symptoms. Basic treatment also involves the intervention of psychological support and proper counseling for effective management of eczema complications. [2, 3]
Standard Treatment
Standard treatment includes the intervention of both systemic and topical agents. It is important to know that topical agents are preferred over systemic agents.
Topical agents:
Topical agents include corticosteroids, anti-infective agents, and calcineurin inhibitors. Topical steroids for eczema management are prescribed based on the severity of symptoms, the extent of disease, and distribution skin lesion distribution of lesions. Short-acting corticosteroids are usually preferred over long-term use of corticosteroids due to multiple side effects. Remember that potent corticosteroids are recommended for highly lignified skin conditions. Corticosteroids such as fluticasone 1- 2 times a week are recommended for eczema symptoms. The potential side effects of topical steroids include the development of acne rosacea, striae, perioral dermatitis, skin atrophy, and adrenal suppression. [2, 3]
Topical calcineurin inhibitors such as Tacrolimus ointments 0.03% and Pimecrolimus cream 1% are used as a secondary drug of choice for eczema management. They act as immunomodulators that inhibit the production of cytokines from activated T-cells and inflammatory cells. It is important to mention that these drugs do not possess health risks for 2-4 years and benefit eczema patients having age ≥two years. [2, 4]
The interventions of anti-histaminic agents such as Chlorpheniramine, Hydroxyzine, and Cetirizine help the concomitant urticaria or concurrent allergic rhinitis associated with eczema. Plus, these agents also ease itching during the night and promote a good night's sleep. The side effects of oral histaminic include drowsiness, impair driving ability, and learning capability. Topical infective agents involve applying antibacterial, antiviral, or antifungal formulations that prevent both aggravations of symptoms and skin infections at the site of itching. The potential adverse event includes the growth of resistant pathogens, including methicillin-resistant S. Aureus, with irrational use of topical antibacterial agents. Medical research studies recommend using fusidic acid/mupirocin ointment for local infections and cephalosporin/ penicillinase-resistant penicillins for extensive superinfections without S. Aureus. In comparison, in the case of viral infections, use systemic antiviral therapy with great care. Moreover, it is advised to use antifungal agents for dermatophyte infections as it aggravates the eczema symptoms. [2, 3]
Systemic Therapy:
Standard systemic therapy has opted when the eczema symptoms are recurring and do not respond to the topical agents. The overview of systemic therapeutic agents is given below.
Cyclosporine: It is an immunomodulator that inhibits cytokine transcription and helps manage severe, refractory atopic eczema. The common disadvantage of cyclosporine is the rapid relapse after abrupt cyclosporine discontinuation. Plus, it can cause kidney or liver impairment, tremors, headache, nausea, myalgias, hyperlipidemia, paresthesia, gingival hyperplasia, and high blood pressure. [2, 3]
Systemic Glucocorticoids (Steroids): It helps temporary suppression of eczema symptoms. They are temporarily prescribed for short-term use to control eczema flares. It is advised to gradually discontinue the systemic steroid use once the symptoms subside. Don't stop the steroids use abruptly to prevent the risk of eczema flare-up or rebound. Side effects of glucocorticoids are gastric ulcer, Cushing syndrome, diabetes, osteoporosis, hypertension, and glaucoma. [2, 3]
Antimetabolites: Antimetabolites include Mycophenolate mofetil, Methotrexate, and Azathioprine that help the management of refractory eczema. They are also recommended for resistant pathogens and improve eczema symptoms. It is advised to carefully monitor herpes retinitis, and dose-related bone marrow suppression with antimetabolites use. Side effects of antimetabolites include Liver dysfunction, headache, fatigue, gastrointestinal complaints, gastrointestinal disturbances, pulmonary toxicity, liver dysfunction, and leucopenia. [2, 3]
Interferon-γ: Interferon-γ reduces IGE levels and decreases the expression of th2 cells that help manage severe eczema conditions. They are usually safe for twelve weeks, but they can cause certain side effects, including fever and headache in the initial stage of administration. [2, 3]
Phototherapy: It involves the intervention of natural sunlight as a secondary option in eczema symptoms management. Phototherapy helps both acute and chronic cases of eczema. It uses UVA-1 of 340-400 nm wavelength light for acute cases and UVB of 311 nm wavelength light for chronic cases. UVA radiation may target the epidermal Langerhans cells and eosinophils. In comparison, the UVB radiations act as immunosuppressants and support eczema management. It is advised to carefully consider the phototherapy intervention for skin pain, pigmentation, cutaneous malignancies, pruritus, and erythema. [2, 4]
Allergen immunotherapy: It is another approach toward eczema management that involves the intervention of subcutaneous and sublingual immunotherapies. However, there are not enough studies about its effectiveness. Also, patients show poor compliance with allergen immunotherapies. [2, 3]
Biologics: Studies also reported the beneficial effects of various biologics in the management of eczema symptoms. These include Rituximab, Omalizumab, Pitrakinra, Dupilumab, Infliximab, Mepolizumab, and Tocilizumab or Atlizumab. However, future studies are needed to conclude final remarks about their safety and efficacy in eczema treatment. [2, 3]
Adjunct treatment involves the use of natural remedies, including herbs and supplements, to ease eczema symptoms. These remedies include primrose oil, omega-3, Vit D, Probiotics, and Korean red Ginseng. Different studies reported significant positive effects of these remedies in eczema symptoms management compared to placebo. However, extensive studies are needed to define their roles and effectiveness in eczema treatment. [2]
Studies also reported the use of following natural remedies for eczema symptoms management. [5, 6]
Long term Use of Steroids for Eczema Symptoms:
The long-term use of steroids, both topical and systemic formulation, possesses harmful effects. It is advised not to use steroids for a more extended period in the treatment of eczema symptoms. The long-term use of topical steroids increases the risk of skin discoloration, thin spidery blood vessels, bruising and may develop permanent stretch marks (striae).
Plus, they can also aggravate the symptoms of other skin conditions, including acne, perioral dermatitis, and rosacea. Moreover, the use of systemic corticosteroids for the long term favors the development of morbidities, including local skin atrophy and other side effects. These side effects include Cushing syndrome, diabetes, high blood pressure, glaucoma, gastrointestinal symptoms, and osteoporosis. Thus, the corticosteroids use for a longer term is not safe in the management of eczema symptoms. [3, 7]
Need my help treating your eczema beyond the anti-inflammatory and hormone balancing nutrition in my "Hormonal Acne Diet Program"? Simply visit my SCHEDULE page to treat yourself to a Holistic Dermatology visit!
Dr. Nicole Sundene, NMD
Dr. Sundene is a Naturopathic Doctor in Scottsdale, Arizona, and is considered a Female Hormone Expert in Women's Health and Bioidentical Hormones. She specializes in Holistic Women's Health for Menopause, Thyroid, Hashimotos, PMS, Perimenopause, Autoimmune, Postpartum, Chronic Fatigue, Depression, Anxiety, Food Allergies, Digestion, Dermatology , Acne, Psoriasis, Eczema and Adrenal Hormonal Conditions. In 1999 she began working for a Hormone Doctor prior to starting Naturopathic Medical School. With over 22 years of experience in both Prescription and Natural women's health and hormones she presents to women the best integrated health solutions for their Chronic Disease. She has been an Herbalist for over 27 years and enjoys teaching women how to use herbs to balance their hormones, nutrition and optimize their health. Dr. Sundene relies on blood testing for her hormone metrics. The hormone testing is covered per the patient's insurance plan and conducted at certain points in the woman's menstrual cycle. To learn more about Hormone Testing for Women Visit: Bioidentical Hormones. Follow Dr. Sundene on Instagram, Twitter and Facebook for more tips on Women's Health, Female Hormones and Naturopathy!
References:



[…] Dermatitis, itchy scalp, scalp eczema and psoriasis are so annoying they drive patients in droves to see me as a Naturopathic Doctor that […]
I am so thankful I found you to finally fix my eczema! If you have eczema you need to get it treated with Naturopathy!!